
TM
833.527.8777
833.KC.SUPPS
NUTRACEUTICALS, LLC

StabliEyez Corneal Protection Formula for Keratoconus (90 Capsules)
(In Stock)
$59.99 USD
The ONLY Supplement Company that Meets Your Unique Nutritional Needs as a Patient With Keratoconus

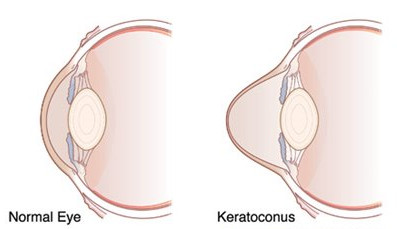

WHAT IS KERATOCONUS AND HOW WILL STABILEYEZ HELP ME?
Keratoconus is a non-inflammatory thinning of the cornea that causes it to bulge into a cone-like shape. This distortion of the natural shape results in blurry vision, usually from a combination of increasing nearsightedness (myopia) and something called irregular astigmatism. It is this irregular astigmatism that causes the largest visual difficulties in correcting the vision in a keratoconic patient. It is also why the above It is also why the various contact lens options are so effective and potentially life changing. Keratoconus tends to start to show up in the teenage years and levels off after the age of 40. People may not even know they have it in the early stages. Although keratoconus always seems to be worse in one eye, it is usually a condition that occurs in both eyes.
When keratoconus progresses, vision becomes very blurry and distorted. Vision worsens because as the cornea bulges forward, irregular astigmatism and nearsightedness develop. As the condition progresses, corneal scarring may occur, causing further vision loss. Some patients with keratoconus notice vision fluctuating frequently while others only see changes over a period of years. People with keratoconus often complain that vision is not improved much with corrected eyeglasses. In some cases, the cornea can bulge forward and become so thin that scarring develops, further impeding vision. In rare cases, the cornea can break down, causing severely reduced vision or even blindness.The exact cause of keratoconus is a bit of a mystery.
It is believed that some people have a genetic defect that causes certain protein fibers in the cornea to split and become weak. These fibers act to hold the cornea together maintaining its clear, dome-like structure. When these fibers become weak, the cornea begins to bulge forward. Some scientists believe that genetics play a strong role in keratoconus because, occasionally, a relative will also develop keratoconus.
People with keratoconus tend to have allergies, specifically atopic allergic diseases such as severe seasonal allergies, asthma, eczema, and food allergies. Interestingly, many patients that develop keratoconus have a history of vigorous eye rubbing. Some of these people have allergies and some don’t, but they tend to rub their eyes. It is thought that this vigorous eye rubbing can cause damage to the cornea, causing keratoconus to develop. Another very popular belief about what causes keratoconus is oxidative stress. For reasons that are still somewhat unclear, people who develop keratoconus have a decrease in antioxidants within the cornea. When the cornea does not have enough antioxidants, the collagen fibers within the cornea split and becomes weak. As a result, the cornea begins to bulge forward. Oxidative stress can be caused by excessive ultraviolet exposure and genetic factors.
Because of the age of onset of keratoconus, it is thought that hormones can play a large role in its development. It is common for keratoconus to develop after puberty. It has also been documented to advance or progress in pregnant women or when people experience significant weight gain or loss. Oftentimes, people with early keratoconus first develop astigmatism. Astigmatism is caused by the cornea having an oblong shape, like a football, instead of a spherical shape, like a basketball. A cornea with astigmatism has two curves, one flat curve, and one that is steep. This causes images to appear distorted in addition to appearing blurry. However, these patients tend to come back into their optometrist’s office a little more frequently, complaining that their vision seems to have changed. Because the cornea gradually becomes steeper, nearsightedness is also frequently diagnosed. Nearsightedness causes objects to become blurry at a distance.
When a rigid lens of any type is placed on the cornea, it immediately corrects the shape distortion of the keratoconus by providing a smooth, regular and optically flawless surface to the keratoconic cornea. Since most of the structures of the eye other than the cornea are normal and healthy, the resulting vision is usually excellent. Keratoconus is variable in its progression and one eye is almost always significantly worse than the other. Some people hardly change over time and about 15% progress to corneal transplantation.
In recent years another treatment has proven effective in slowing progression in those that are changing rapidly. Collagen crosslinking (CXL) is a treatment where the outer layer of the cornea is removed and a solution containing Vitamin B2 is applied to the surface of the eye. An ultraviolet (UV) light is then shown on the cornea. This results in a strengthening and stiffening of the corneal collagen and a slowing of the corneal thinning. It is important to note that none of these surgical treatments are effective at correcting vision and are more aimed at controlling the disease. Contact lenses are almost always necessary to reach your ultimate visual potential. Usually by about age 40, keratoconus gets more stable and large changes later in life are unusual.
A Word From Dr. Scheno
For over 25 years, I have seen patients with keratoconus and other corneal issues. On a daily basis, I would be asked, "Is there anything that I can take or food I should eat for my keratoconus that would potentially help my condition and vision to not get worse?" Until recently, my answer was unfortunately not. There was never a product available that focused on the main issue in keratoconus which is oxidative stress (OS) that I could recommend even as study after study showed that OS was primarily responsible for the vision changes, scarring and disease progression that we routinely see in keratoconus. So realizing this, I set out to develop a formulation of my own that would possess the necessary antioxidant nutrients that the cornea needs to support its efforts to overcome OS, while still being affordable and of the highest quality. Thus Stabil-Eyez was born. I began recommending them to patients in my office and then subsequently introducing them to a broader audience yearning for a dietary supplement that is tailored strictly to the unique metabolic needs of the cornea in keratoconus patients. In its first year of release, it is still the first and only supplement of its kind and has earned worldwide accolades from doctors and patients alike. I ask you to try our product. I am sure you will find that it helps support corneal health and ultimately to help preserve your vision and quality of life.